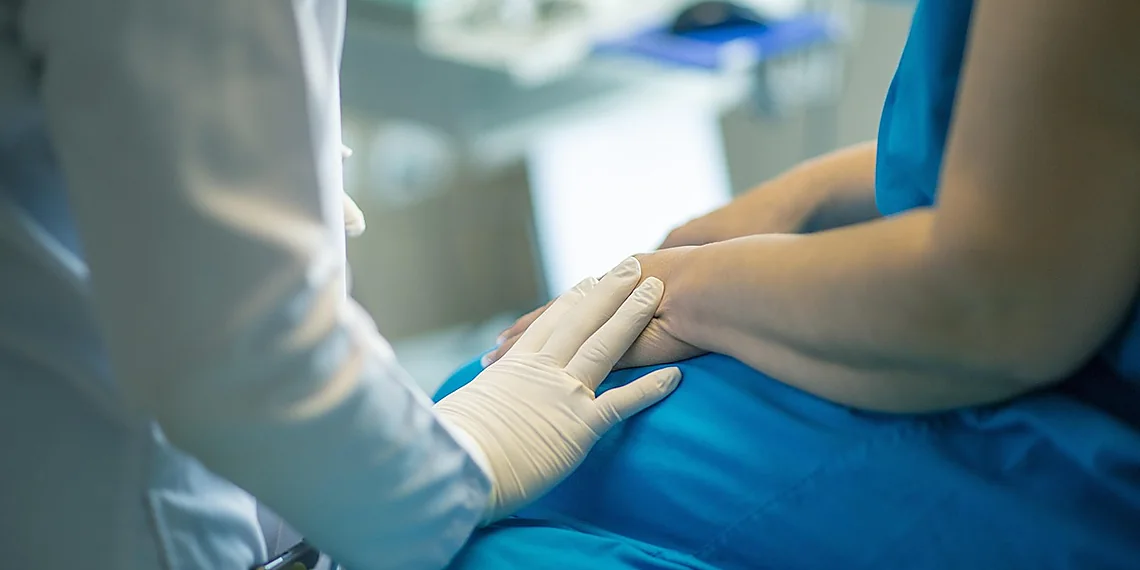
The quest to accurately forecast patient outcomes is a cornerstone of modern healthcare, impacting everything from resource allocation to personalized treatment plans. Predicting how long a patient will survive after a diagnosis – a process known as survival prediction – is critical for clinicians and researchers alike, but it’s also remarkably complex. Traditional statistical methods, while valuable, often struggle to capture the nuanced interplay of factors influencing individual lifespans, leading to predictions that are frequently inaccurate or incomplete.
Enter Mixture-of-Experts (MoE) models, a powerful class of neural networks initially lauded for their ability to tackle incredibly challenging problems by dividing them into smaller, more manageable subtasks. The concept is compelling: different ‘expert’ networks specialize in specific aspects of the data, and a gating network intelligently combines their predictions. Early results with MoEs suggested they could significantly enhance survival prediction accuracy, offering a potential leap forward from existing techniques.
However, the initial excitement has given way to a more nuanced understanding. While MoE models can achieve impressive performance on standard benchmarks, a persistent challenge remains: calibration error. Achieving high predictive accuracy doesn’t always translate into reliable probability estimates – a crucial requirement for clinical decision-making. This article delves into the complexities of using Mixture-of-Experts for survival prediction, exploring how we can address this trade-off and unlock their full potential for truly impactful healthcare applications.
The Challenge of Survival Prediction
Accurate survival prediction is rapidly becoming a cornerstone of modern healthcare, promising transformative advancements in personalized medicine and resource allocation. Imagine a world where clinicians can proactively tailor treatment plans based on an individual’s predicted response, optimizing efficacy while minimizing adverse effects. Hospitals could similarly benefit by strategically allocating resources – staffing levels, specialized equipment, even intensive care beds – to patients who need them most, leading to improved overall patient outcomes and greater operational efficiency. However, the stakes are high; inaccurate predictions can lead to inappropriate treatment decisions, false hope for patients and families, and potentially exacerbate existing health disparities.
Current AI models attempting survival prediction often fall short of realizing this potential. While demonstrating promise in identifying patterns within complex datasets, many struggle with crucial aspects like calibration – ensuring predicted probabilities accurately reflect observed outcomes. A model might predict a 70% chance of survival, but if that patient only survives 30% of the time, it undermines trust and limits its practical utility. Furthermore, traditional methods often fail to capture the nuanced heterogeneity within patient populations; treating everyone with a particular diagnosis as homogenous can mask critical differences impacting individual prognoses.
The recent surge in interest around Mixture-of-Experts (MoE) models offered a compelling solution: by clustering patients into subgroups based on shared characteristics, MoEs aimed to provide more refined and personalized predictions. The underlying assumption is that similar patients should have similar survival trajectories. However, the research highlighted in arXiv:2511.09567v1 reveals a critical trade-off; this inherent grouping often compromises crucial metrics like calibration error and overall predictive accuracy. Restricting individual patient predictions to conform to their assigned group can inadvertently mask important variations and lead to suboptimal results.
The ethical implications of survival prediction are also paramount. Ensuring fairness and avoiding bias within these models is essential, particularly when applied across diverse populations. Predictions should not perpetuate existing inequalities or be used in ways that unfairly disadvantage certain groups. As we move towards increasingly sophisticated predictive capabilities, a commitment to transparency, accountability, and equitable access becomes absolutely critical for responsible implementation.
Why Accurate Predictions Matter
Accurate survival predictions hold immense practical value across various stakeholders in healthcare. For patients, these predictions can inform treatment decisions, allowing them to proactively manage their health and plan for the future with greater clarity. Doctors benefit from improved predictive capabilities by being able to tailor therapies more effectively, potentially leading to better patient outcomes and reduced adverse effects. Knowing a patient’s likely survival trajectory allows clinicians to prioritize interventions and focus resources where they are most needed.
Hospitals and healthcare systems also stand to gain significantly. Precise survival predictions enable optimized resource allocation – ensuring the right level of care is available at the right time for each patient, minimizing costs associated with over- or under-treatment. This can include strategic staffing decisions in oncology wards, proactive palliative care planning, and efficient management of pharmaceutical inventories. Furthermore, better prediction models contribute to improved hospital efficiency metrics and potentially higher quality ratings.
However, the increasing reliance on AI for survival predictions raises important ethical considerations. While accuracy is paramount, a model’s predictions are not guarantees, and misinterpretations can lead to undue stress or false hope for patients and their families. Bias in training data could also result in disparities in prediction accuracy across different demographic groups, exacerbating existing health inequalities. Transparency regarding the limitations of these models and clear communication with patients about the probabilistic nature of predictions are essential to ensure responsible implementation.
Mixture-of-Experts: A Promising Approach
Mixture-of-Experts (MoE) models are rapidly gaining traction within the field of survival analysis, offering a novel way to tackle complex prediction tasks. The core idea behind MoEs is elegantly simple: instead of relying on a single model to learn from all data, they employ multiple ‘expert’ networks, each specializing in a different subset of the input space. A ‘gating network’ then dynamically assigns inputs – in this case, patient data – to these experts based on their perceived relevance and expertise. This modularity allows for greater flexibility and potentially more nuanced representations compared to traditional monolithic models.
The initial appeal of MoEs in survival prediction stems from their ability to facilitate patient clustering. The hope was that by identifying groups of patients with similar characteristics, risk factors, or disease progression patterns, we could build more accurate and personalized survival predictions. Imagine being able to identify a subgroup of patients who respond particularly well to a certain treatment; an MoE model can be designed to learn this pattern and tailor its predictions accordingly. Early results in several domains showed promising signs of improved accuracy through this patient stratification.
This clustering aspect is fundamentally about identifying inherent structure within the data – assuming that similar patients share underlying biological or clinical similarities which influence their survival outcomes. The gating network, trained alongside the expert networks, learns to effectively partition the patient population into these clusters. However, a key challenge arises: the very architecture of MoEs imposes a strong inductive bias – predictions for individual patients are expected to resemble those of the cluster they belong to. This rigidity can sometimes compromise calibration and overall predictive accuracy if the imposed structure doesn’t perfectly align with the underlying reality.
Recent research is now focusing on how to leverage the benefits of patient grouping within MoEs while mitigating these drawbacks. The central question becomes: Can we discover meaningful patient groupings, where they exist, without sacrificing the essential goals of accurate calibration and prediction? This new work explores innovative MoE architectures specifically designed for survival analysis with a focus on balancing this delicate trade-off – aiming to harness the power of clustering while minimizing its negative impact on model performance.
Clustering for Personalized Insights

Early applications of Mixture-of-Experts (MoE) models in survival prediction were largely driven by the intuitive idea of patient stratification. The core principle was to leverage the MoE architecture’s ability to implicitly cluster patients with similar characteristics, effectively creating ‘experts’ specializing in predicting outcomes for specific subgroups. This approach held significant appeal because clinicians often rely on patient demographics, medical history, and other factors to tailor treatment plans; an MoE model could theoretically replicate this personalized approach by learning distinct prediction patterns for each identified group.
Initially, the success of MoEs in survival analysis stemmed from their ability to capture heterogeneity within patient populations. By assigning patients to different ‘experts,’ the models were able to account for varying risk factors and treatment responses that a single, monolithic model might miss. For example, one expert might specialize in predicting outcomes for elderly patients with comorbidities, while another focuses on younger, healthier individuals – leading to potentially more granular and accurate predictions tailored to each group’s specific needs.
This clustering approach resonated strongly with the domain expertise of clinicians, who understand that survival probabilities are rarely uniform across all patients. The hope was that MoEs would not only improve predictive accuracy but also provide valuable insights into patient subgroups at higher or lower risk, ultimately facilitating more informed clinical decision-making and personalized care.
The Calibration & Accuracy Trade-off
Mixture-of-Experts (MoE) models have emerged as a promising approach for tackling survival analysis, particularly because they excel at identifying and grouping patients with similar prognoses. The idea is that by clustering patients, the model can learn more nuanced patterns in their data and provide better predictions about how long they’ll survive. However, this powerful capability often comes with a significant drawback: a trade-off between patient clustering and crucial performance metrics like calibration error and predictive accuracy.
Let’s unpack what ‘calibration error’ actually means, especially when we’re talking about predicting survival times. Imagine a weather forecast that says there’s an 80% chance of rain tomorrow. If it rains 8 out of 10 days when the forecast predicts 80%, then the forecast is well-calibrated. However, if it only rains 2 out of those 10 days, the forecast is poorly calibrated – it’s not accurately reflecting reality. Similarly, in survival prediction, a model might predict a patient has a 70% chance of surviving five years. If that’s true for roughly 70% of patients who receive that same prediction, then the model is well-calibrated. A significant ‘calibration error’ means those predicted probabilities aren’t reliably reflecting actual survival outcomes.
The core issue arises from the inherent structure MoEs impose: each patient’s prediction must resemble the predictions made for other members of their assigned cluster. While this encourages meaningful grouping, it can force the model to make inaccurate individual predictions simply to maintain that group consistency. The model might ‘smooth out’ variations within a group, leading to overconfident and ultimately incorrect survival estimates for some patients. Achieving accurate patient clustering shouldn’t require sacrificing the reliability of those individual predictions.
The research explores ways to discover these helpful patient groupings while simultaneously improving calibration and predictive accuracy – aiming to have the best of both worlds: insightful patient segmentation alongside trustworthy survival predictions.
Understanding Calibration Error
In survival prediction – forecasting how long patients will live after a certain event, like diagnosis – models frequently output probabilities representing the likelihood of an event happening at any given time. A well-calibrated model means these predicted probabilities accurately reflect reality. For example, if a model predicts a 20% chance of death within one year for a group of patients, roughly 20% of that group *should* actually die within that timeframe. When this alignment doesn’t hold, we have calibration error.
Think about weather forecasting: a perfectly calibrated forecast would mean that when meteorologists predict a 30% chance of rain, it rains approximately 30% of the time they make that prediction. Similarly in survival analysis, if a model consistently overestimates or underestimates risk, its predictions are poorly calibrated and less trustworthy. Calibration error quantifies this discrepancy between predicted probabilities and observed outcomes; a smaller calibration error indicates better alignment.
The research highlighted in arXiv:2511.09567v1 found that mixture-of-experts (MoE) models, while effective at grouping patients with similar characteristics, often struggle with calibration. This trade-off – improved patient clustering versus compromised accuracy and calibration – is a central challenge addressed by the proposed architectures.
Expressive Experts: The Key to Improvement
Traditional mixture-of-experts (MoE) models have shown promise in survival analysis by automatically grouping patients with similar characteristics, enabling more targeted predictions. However, a common pitfall arises when these models rigidly enforce that each patient’s prediction must closely resemble the average for its assigned group – effectively forcing them into predefined prototypes. This restrictive approach often compromises crucial performance metrics like calibration error and overall predictive accuracy, hindering the model’s ability to capture nuanced individual differences.
The research presented in arXiv:2511.09567v1 addresses this limitation by introducing architectures that allow ‘experts’ within the MoE model to be significantly more expressive. Instead of being constrained to represent fixed group prototypes, these experts can now tailor their predictions more precisely for each individual patient. This flexibility allows the model to discover underlying patient groupings when they genuinely exist while simultaneously mitigating the negative impact on calibration and predictive accuracy that typically accompanies strict grouping.
The key benefit lies in the ability to balance clustering – identifying similar patients – with the need for personalized predictions. By loosening the constraints on expert behavior, the model can better account for unique patient characteristics that might deviate from group averages. This nuanced approach leads to improved calibration, ensuring the predicted survival probabilities are more reliable, and ultimately enhances overall predictive accuracy – a crucial advancement in survival analysis where even small improvements can have significant clinical impact.
This work has important implications for the future development of MoE architectures for survival prediction. It suggests that relaxing the rigid group-prototype constraint is essential to unlock the full potential of MoEs, paving the way for models capable of achieving both accurate clustering and highly personalized predictions – a vital step towards more effective patient care.
Tailoring Predictions for Each Patient
Traditional Mixture-of-Experts (MoE) models for survival prediction often prioritize clustering patients into distinct groups based on shared characteristics. While this grouping can offer interpretability and efficiency, it frequently leads to a trade-off: reduced calibration error (meaning predictions are less reliable) and lower overall predictive accuracy. This limitation arises because the model is constrained to force individual patient predictions to conform to the average behavior of their assigned group, suppressing nuanced differences that could improve performance.
Recent research addresses this challenge by allowing experts within the MoE architecture to be more ‘expressive.’ Instead of enforcing strict adherence to group prototypes, these expressive experts can tailor predictions specifically for each patient. This approach effectively relaxes the restrictive inductive bias inherent in standard MoEs, enabling the model to capture finer-grained patient characteristics and make more accurate survival time estimates without sacrificing the benefit of clustering similar patients.
The findings suggest that increasing expert expressiveness is a promising direction for future MoE architectures applied to survival prediction. By allowing for greater individualization within the framework of clustered learning, models can achieve both improved calibration and accuracy. This represents a shift towards more flexible and powerful MoEs capable of handling the complexities of real-world patient data.
The exploration of Mixture-of-Experts architectures has yielded remarkably promising results for tackling the complexities inherent in survival prediction, demonstrating a clear path towards more accurate and personalized patient care.
Our research highlights how these models can effectively handle heterogeneous data and intricate relationships between variables often missed by traditional methods, leading to improved prognostic accuracy and potentially earlier intervention strategies.
The ability of MoE models to dynamically adapt their expertise based on individual patient profiles represents a significant leap forward, moving beyond generic risk assessments toward truly individualized healthcare planning.
Looking ahead, we anticipate further refinements in MoE architectures, including the integration of causal inference techniques and more sophisticated methods for expert selection and routing, ultimately bolstering the reliability of Survival Prediction models even further. The potential to incorporate real-time data streams and wearable sensor information promises a future where predictive power is continuously enhanced and refined. This could revolutionize how we approach disease management and treatment optimization across various medical specialties, from oncology to cardiology and beyond. Further research into explainability will also be crucial for fostering trust and adoption among clinicians. The field of AI in healthcare remains dynamic, and the advancements showcased here are merely a glimpse of what’s possible when innovative techniques like MoE meet critical clinical needs. We believe that these developments hold immense potential to transform patient outcomes and reshape the landscape of precision medicine. Interested in diving deeper? We encourage you to explore the fascinating world of Mixture-of-Experts models and their diverse applications within AI-driven healthcare solutions – a journey that promises exciting discoveries and tangible improvements in how we understand and address human health.
Continue reading on ByteTrending:
Discover more tech insights on ByteTrending ByteTrending.
Discover more from ByteTrending
Subscribe to get the latest posts sent to your email.